
As I am sure you have heard, leading health organizations, including the WHO and CDC, are focused on addressing the spread of Zika virus. This blog piece is intended to help travelers to Ecuador and the Galapagos understand their risk, which can be low, and provide information on precautions that can be taken to avoid contracting Zika. The real concern surrounding Zika has been directed toward the suspected link between the virus and a severe birth defect know as microcephaly, which will be addressed at the end of this blog.
Understanding How Zika Virus Can Affect Your Trip
A key way for travelers to manage their risk concerning Zika is in understanding that the virus is primarily transmitted to people via mosquito bites, which is why the following information is important:
The Ecuadorian Ministry of Health recently reported that Zika is occurring in the country at elevations below 1,200 meter (3,937 ft). It's easy to avoid these lower elevations in Ecuador simply by flying into Quito at 2,850 meters (9,350 ft) above sea level. The fact that the surrounding highlands stand at 9,000 ft and up has made both Quito and its high elevation surrounds immune from other mosquito born afflictions such as malaria. The CDC reports, for example, that malaria is not known to occur in the Ecuadorian highlands.
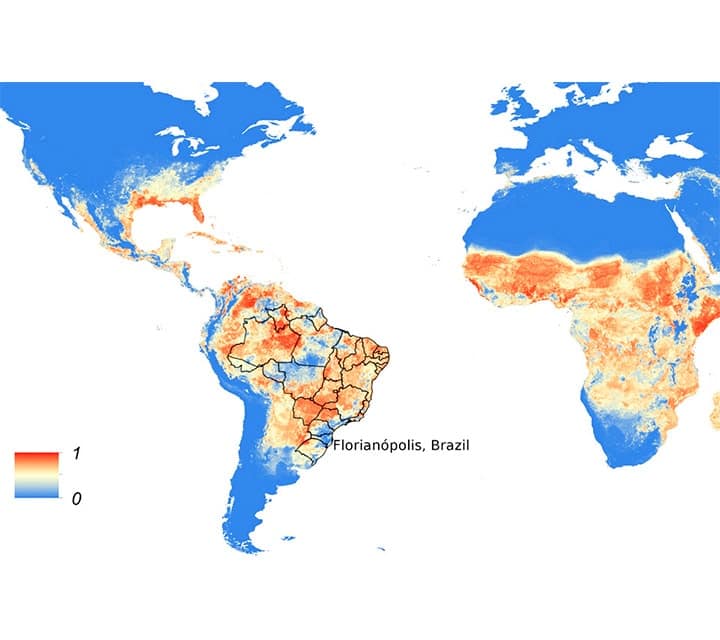
The Galapagos is another place the CDC reports as being malaria free. A reason for this is that the Galapagos offers a marine desert environment where one rarely sees mosquitoes. Even in the more lush highland one sees few mosquitoes. While El Niño may temporarily increase the mosquito population in the islands, this should be short lived. Another factor is that the Galapagos National Park has check points set up to prevent introduced species from entering the islands. The population in the Galapagos is small with only 4 inhabited islands. Floreana, for example, has a population of roughly 100 people, while Santa Cruz has roughly 12,000 at the other end of the spectrum. The fact that Zika doesn't remain in the blood of a person once they recover, combined with the Galapagos' small population means the disease will likely not gain a permanent foothold there.
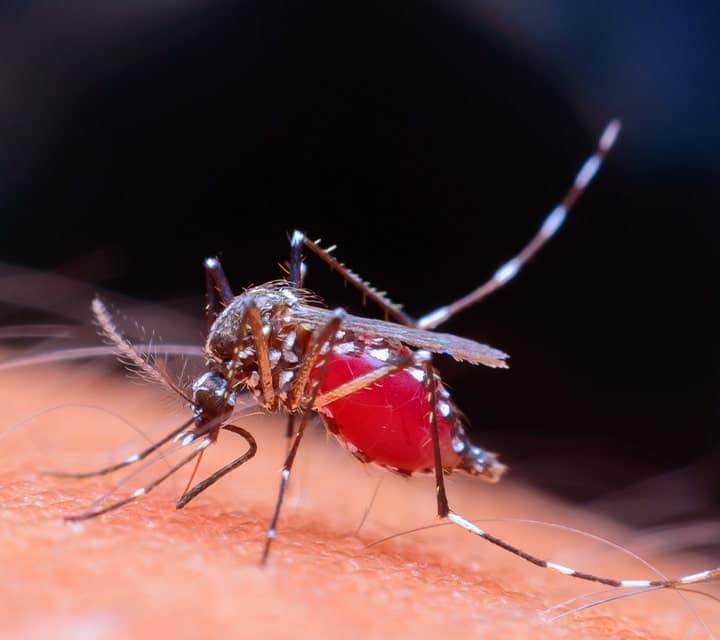
The risk of contracting Zika is therefore low for travelers who stick to the Ecuadorian highlands and Galapagos, which one can easily do on a Galapagos adventure. The risk is higher at lower elevation areas, particularly along the Ecuadorian coast, which is not generally a tourist area, as well as the Amazon, which is. One can simply avoid these areas of higher risk to lower the chance of contracting Zika.
For those who still would like to visit the Amazon, like other insect born diseases, one of the best preventions for Zika virus is to avoid mosquito bites. The CDC offers a wealth of information on Zika as well as prevention at this link.
The CDC also reports instances of Zika being transmitted sexually and provides information on sexual transmission and prevention at this link. Fortunately CDC also reports, “Zika virus usually remains in the blood of an infected person for only a few days to a week. The virus will not cause infections in an infant that is conceived after the virus is cleared from the blood. There is currently no evidence that Zika virus infection poses a risk of birth defects in future pregnancies.”
It's important to understand that the potential threat to most travelers vs. pregnant women is quite different. For most travelers the CDC reports that, “About 1 in 5 people infected with Zika will get sick. For people who get sick, the illness is usually mild. For this reason, many people might not realize they have been infected...The most common symptoms of Zika virus disease are fever, rash, joint pain, and conjunctivitis (red eyes). The illness is usually mild with symptoms lasting from several days to a week. Severe disease requiring hospitalization is uncommon...”
For pregnant women the considerations are different, "Until more is known, CDC recommends special precautions for pregnant women and women trying to become pregnant,” which one can read at this link.
The current alarm surrounding Zika is focused on the suspected link between the virus and the fetal deformity called microcephaly, which affects both brain and skull development. That link surfaced in Brazil, which experienced an abnormally high incidence of both Zika and microcephaly in the latter half of 2015 and beginning of 2016. But the assumed link is undergoing scrutiny. The Guardian reports that "Almost all the linked cases are found in the north-east region of Brazil. Elsewhere, the Zika outbreak does not appear to have had the same impact. In neighboring Colombia, which has more than 31,000 Zika cases, including at least 5,000 pregnant women, there has not been the same sharp rise in fetal deformities... Doubts about the causes continue to spark controversy. This week, the state government of Rio Grande do Sul in the south of Brazil banned the use of the larvicide pyriproxyfen after a report by the Argentinian group Physicians in Crop-Sprayed Towns suggested it might be causing the fetal brain deformities."
Leslie Lobel, chair of the virology department in Ben-Gurion University, who has studied Zika in Uganda, where it was first discovered in 1947 states “It’s not clear that what’s going on in Brazil is linked to the Zika virus. There’s no definitive proof that Zika is causing microcephaly. I believe the hysteria is way ahead of the research or the facts about the pathology surrounding this virus... I don’t want to downplay this. The association is very compelling, very clear. But we need a lot more work and we need to do it fast.” Other reports have asserted that Zika may be linked to Guillain-Barré syndrome, a fairly rare affliction in which a patient's immune system damages nerve cells causing muscle weakness and even paralysis. The CDC reports, " We do not yet know if there is a connection between GBS and Zika virus infection. It is difficult to determine if any particular pathogen or germ “causes” Guillain-Barré syndrome (GBS)."
Ecuador, the Galapagos, Peru, Chile & Zika Virus
At the time of this writing, there have been 3 confirmed Zika cases in Ecuador. There are about 30 people “under observation”. These cases have occurred in the province of Manabi, which is along the northern coast and not a place we send travelers.
Because the Aedes mosquito species is the vector for Zika, a preventative approach is to avoid places where one finds mosquitoes such as the Amazon and some areas along the coast of the Ecuadorian mainland, and of course protect against mosquito bites. Though possible, it is less likely that travelers will contract Zika in the Ecuadorian highlands because one is less likely to encounter mosquitoes at high elevation. It is possible that the disease will eventually spread to the Galapagos but, the National Galapagos Park has fairly strong environmental controls in place that mitigate against this. Typically one does not encounter many mosquitoes in the Galapagos to begin with, though there will more than usual in 2016 due to El Niño. At this writing, Zika has yet to be reported in Peru.

We recommend travelers continue to monitor Zika at the CDC Webiste and, as always, travelers should consult with their healthcare provider before traveling abroad.
Zika will likely continue to spread to low lying, mosquito prone areas of the Americas including the USA. Yet, as research findings replace speculation and media hysteria is replaced by educated action, the risk of visiting the Ecuadorian highlands and the Galapagos will largely remain low, even until the time a vaccine is hopefully developed.
We will be updating this post as we continue to monitor this subject and find any further updates.
Zika Virus Update - 2/8/16:
While we know there is still concern of the Zika Virus that is spreading in South America, Peru has had only one reported case of the virus in a Venezuelan man who contracted the disease while traveling outside of Peru. Peru's Health Minister is taking measures to ensure the virus does not spread in the country. It is the same vector that transmits Dengue and Yellow Fever, two diseases that have been in this part of the world for many years. The symptoms of the Zika Virus are not as severe as Dengue and Yellow Fever, and treatment is just rest and Tylenol, however there is no vaccine or cure for it yet.

Zika Virus Update - 2/15/16:
In Argentina, there have been 3 confirmed cases, but these were “imported”, i.e. people that caught the virus outside of Argentina and came into the country with it in their system. The chances of the virus circulating and increasing independently in Argentina are very low since Argentina offers little in terms of environments where the mosquito can proliferate. However, the Argentinean government is taking measures and educating the population just to be on the safe side.
The situation is similar in Chile, with 3 confirmed “imported” cases. However, in Chile, the government has informed that there is no probability of the disease spreading in the country because the mosquito does not exist in the country’s mainland. The mosquito does exist on Easter Island, but for many years, even prior to the Zika virus issue, the local people population has consistently taken preventive measures (due to the other diseases that the mosquito may carry) and though they had a couple confirmed cases (one in 2013 and one 2014) there has never been an outbreak due to said existing preventive measures.
Zika Virus Update - 3/7/16:
The majority of the new Zika virus cases are native, not imported. This is very different from what we were told originally! Most of these Zika cases are even “suspect” cases, not confirmed. The virus has spread, there’s no doubt about it, though it has not done so by any means as it has in other countries like Brazil, Colombia and Venezuela.
Travel to Ecuador & the Galapagos remains safe, and the usual precautions are advised listed above.
Zika Virus Update - 11/22/16:
The mosquito-borne Zika virus will no longer be treated as an international medical emergency, the World Health Organization (WHO) has declared. The WHO will now shift to a longer-term approach against the infection, which has spread across Latin America, the Caribbean and beyond. The pandemic has basically stopped, at least as an “emergency”. The Zika Virus has basically been controlled for now and that traveling is “back to normal” with the exception of pregnant women or women looking to get pregnant until “a vaccine is developed”.
* Paul Edward Schicke previously served as Executive Director of the World Initiative for Science & Healthcare, a non-profit dedicated to providing HIV/AIDS testing, prevention and treatment to rural sub-Saharan Africans via mobile clinics.















